Chronic gastritis – causes, side effects and treatments at NaturalPedia.com
Thursday, February 15, 2018 by Ralph Flores
http://www.naturalpedia.com/chronic-gastritis-causes-side-effects-and-treatments-at-naturalpedia-com.html
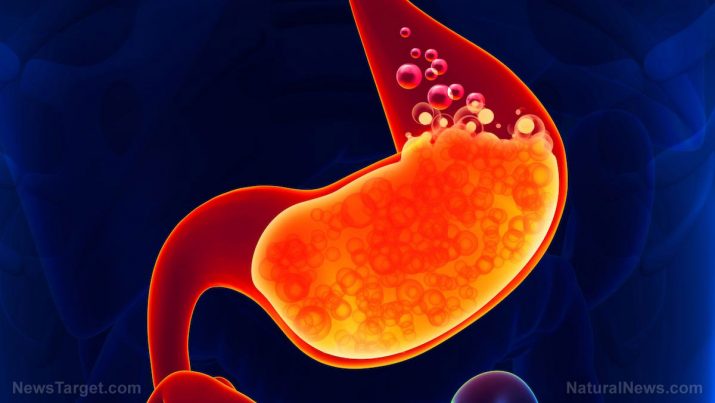
A condition wherein a person’s stomach lining (also called the mucosa) is inflamed or swollen is usually called gastritis. The disease primarily affects the stomach lining, which produces stomach acid and an enzyme called pepsin. These two are responsible for digestion, with pepsin breaking down proteins into units called peptides, which enter the bloodstream or are processed by the pancreas. As this process is highly acidic (it has a pH level of 1.5 to 2.5), the stomach is lined with a thick layer of mucus to protect the tissues from being digested.
If a person has gastritis, the mucosa makes less acid and pepsin. However, this also means that it produces less mucus, which makes the stomach tissue prone to injury.
The condition is usually classified between acute and chronic:
- Acute gastritis is described to be a sudden occurrence and only lasts for a short time.
- Chronic gastritis is recurring and usually lasts for a long time if it is not addressed.
While the term gastritis was first used in 17th-century Germany to describe “the inflammation of the inner lining of the stomach,” it was only considered a tissue-related finding and not a disease. However, this all changed with the discovery of the Helicobacter pylori bacteria in 1982, which opened the door for further classification of chronic gastritis.
Today, the gastritides are classified based on their underlying cause and their histopathologic pattern.
- Type A gastritis, also known as autoimmune atrophic gastritis, happens when the immune system attack healthy stomach cells. This may lead to vitamin deficiencies, anemia, and gastric cancer.
- Type B gastritis is caused by the H. pylori, a gram-negative bacteria that infects the stomach. The bacteria are the “first formally recognized bacterial carcinogen,” and conditions from this type of gastritis can lead to cancer and stomach and intestinal ulcers.
- Type C gastritis occurs with chemical irritants such as nonsteroidal anti-inflammatory drugs (NSAIDs), alcohol, or bile.
H. pylori-related complications are the leading cause of gastritis, with at least 50 percent of the global population known to be infected by the bacteria. Other causes include the following:
- Infections – Bacteria strains such as Helicobacter heilmannii, as well as parasites such as the threadworm, flatworm, and tapeworm, can cause chronic gastritis. It can also be acquired from viral infections like that from cytomegalovirus (CMV) or herpesviruses.
- Gastric infections – This includes granulomatous gastritis, a condition caused when the immune system traps substances in the granuloma, but it is unable to eliminate them.
Known risk factors and symptoms of chronic gastritis
Due to the prevalence of H. pylori, chronic gastritis can affect a wide range of people. However, other risk factors increase the likelihood of getting the condition, such as:
- Excessive alcohol and cocaine use
- Regular intake of NSAIDs like aspirin, ibuprofen, and other painkillers
- Stressful events such as a traumatic injury, critical illness, or a major surgery
- An autoimmune response
Other causes of chronic gastritis include Crohn’s disease, a condition that results in the inflammation of the gastrointestinal tract, and sarcoidosis, which causes the formation of abnormal tissue in various organs in the body.
A person gets infected with H. pylori during childhood, but they do not exhibit the symptoms until much later, which could include pain in the upper region of the abdomen, nausea, vomiting, and anorexia. He may also feel full during meals faster (a condition called early satiety) and experience weight loss.
Symptoms of autoimmune gastritis are a result of the body’s inability to efficiently absorb cobalamin. The condition manifests either as megaloblastic anemia (a disease where the bone marrow produces abnormally large red blood cells) and blood clots. In advanced cases, this could progress to nerve death and cognitive damage.
If symptoms of chronic gastritis appear in concert with a preexisting condition such as Crohn’s disease, a person experiences abdominal pain, nausea, and vomiting. This will also impact the intestinal tract and lead to bleeding.
It is recommended to consult with a health practitioner when either vomiting blood accompanies chronic gastritis or excreting bloody stools.
Chronic gastritis increases a person’s risk of developing the following:
- Peptic ulcers
- Polyp growth in the stomach
- Tumor growth, which could be cancerous
In severe cases, the condition may progress to atrophic gastritis, an insidious form of gastritis that destroys the stomach mucosa and increases the risk of gastric cancer.
Body systems affected by chronic gastritis
Chronic gastritis is primarily located in the stomach; however, complications can affect all body systems.
Food items that may prevent and relieve chronic gastritis
Preventing the spread of H. pylori is difficult, as the mechanism of how it is transmitted from person to person is still not fully understood; however, clinicians recommend regular washing of hands – in particular, after using the bathroom and before eating. Moreover, consuming food that has been properly cooked or washed also decreases the likelihood of getting an H. pylori-related gastritis.
When a person has gastritis, the following food items must be avoided:
- Alcohol
- Caffeinated, decaffeinated, and carbonated drinks
- Fruit juices containing citric acid
- Food items that are high in saturated fat
If a person suffers from chronic gastritis as a result of an H. pylori infection, eating a high-fiber diet, as well as foods that have flavonoids, may inhibit the growth of the bacteria.
Treating and managing chronic gastritis
Gastritis, in general, is treated by reducing the amount of acid in the stomach. The procedure allows that stomach lining to recover and treat any underlying cause.
To reduce the amount of acid in the stomach, the following medications are used:
- Antacids: These have three different salts – magnesium, aluminum, and calcium – as well as compounds like hydroxide and bicarbonate ions that neutralize stomach acid. However, the magnesium salt content of antacids can cause diarrhea, and the aluminum salt causes constipation.
- H2 blockers decrease acid production.
- Proton pump inhibitors (PPIs) are touted to decrease acid production better than H2 blockers.
If the underlying cause is H. pylori, antibiotic treatment is administered regardless if there are other symptoms. Aside from curing gastritis, this decreases the likelihood of more serious complications, such as cancer and peptic ulcers, later on.
When the gastritis is a result of NSAID usage, the healthcare provider may adjust the dosage, change the medication, or discontinue it altogether. In serious cases, such as gastritis caused by stress or an autoimmune response, medications will also be provided to protect the mucosa.
Where to learn more
- Simple Home Remedies for Gastritis
- 5 Natural Juices For Gastritis; How to Make These?
- Strawberries can help cure gastritis
- A Safe and Natural Way to Treat H. Pylori
- Home Remedies for Gastritis – Top 15 Natural Treatments
Summary
Chronic gastritis is a long-term inflammation of the stomach lining. While H. pylori infection is one of the leading causes, it can also come as a result of NSAID usage or an autoimmune response. If left untreated, it could result in severe complications; however, it can be managed through proper diet and lifestyle changes.
Sources include:
Tagged Under: Tags: chronic gastritis





